Evaluation and Management (E/M) Coding: Guidelines and Best Practices for Physicians
Nobody wants to be underpaid. No reasonable person will overbill his services. Everyone desires timely payments. So is it with physicians and providers. However, some physicians and providers don’t receive accurate and timely payments for the furnished services. It's because of the physician's failure to bill the correct level of care.

The OIG report 2010 found that 42% of claims per year for Evaluation and Management (E/M) services were incorrectly coded, which included both upcoding and downcoding (i.e., billing at levels higher and lower than warranted, respectively), and 19% were lacking documentation.
The underlying problem for wrong billing is two-fold:
- Lack of understanding on how the coding system for evaluation and management (e/m) works.
- Inaccurate and incomplete documenting to support the code.
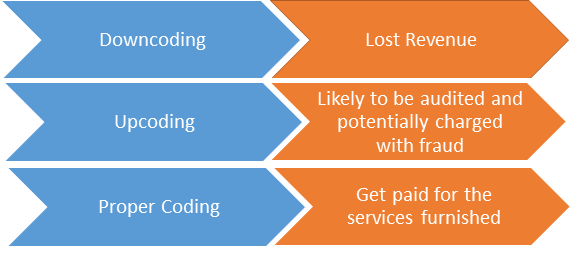
Physicians who find EM coding challenging, must review the basics of EM and understand how to choose the correct Current Procedural Terminology (CPT) code for an e/m visit.
E/M coding System Process
E/M coding translates physician-patient encounters into a five-digit current procedural terminology (CPT) codes to facilitate billing. CPT codes are submitted to insurers for payment. There are individual CPT codes for each billable procedure.
- Accurate Documentation and Billing Requirements & Obligations
- The correct level of billing can be achieved only if the physician documents the medical records accurately and adequately at each patient encounter. Many physicians usually undercode or upcode because they don't understand these rules.
- As Payers have a contractual obligation to enrollees, they may require reasonable documentation that the services are consistent with the insurance coverage provided. 'They may request information to validate the site of service, the medical necessity and appropriateness of the diagnostic and/or therapeutic services provided; and/or that the services reported have been adequately reported.' Says the Evaluation and Management Services .
- Have a billing specialist or alternative source review the provider’s documents before submitting the claim to the payer.
- Providers must make sure that the services provided are properly reflected in the claim submitted.
- E/M Documentation Principles
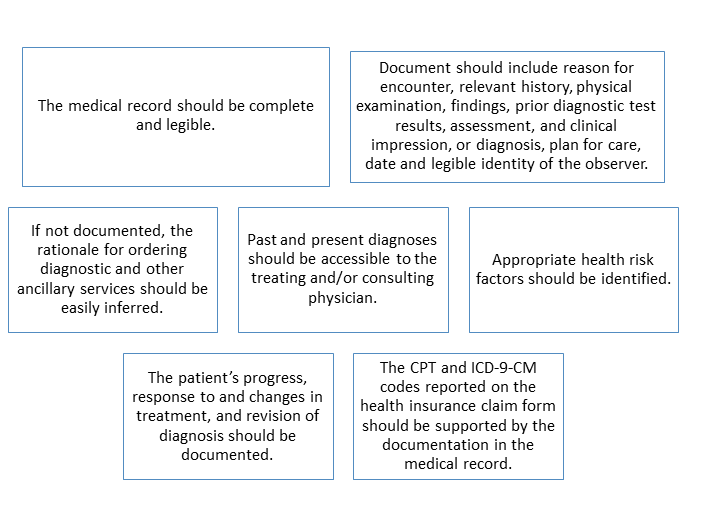
Figure 1General Principles of Medical Record Documentation
To download the detailed E/M guidelines, 1995 click here , and 1997 click here .
To download the claims processing manual for Physicians, nonphysician Practitioners, click here .
3 Components of E/M Documentation
The 3 components are History, Physical Examination, and Medical Decision Making. Below is a brief of each of the components:
History:
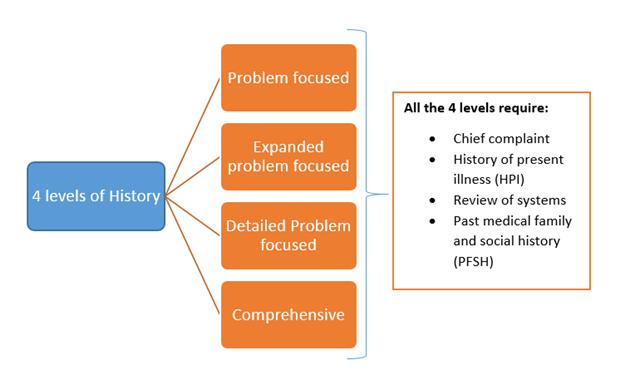
Physical Examination:
Should provide the details of levels of physical exam – problem focused, expanded problem focused, detailed, and comprehensive. The rules for the various levels of physical exam requires the physicians to the exam using specific bullets. Refer page 10 to 41, 1997 E/M.
Medical Decision Making (MDM):
As MDM reflects the intensity of the cognitive labor performed by the physician, it is by far the most important of the 3 components.
The MDM is determined by using the below table:
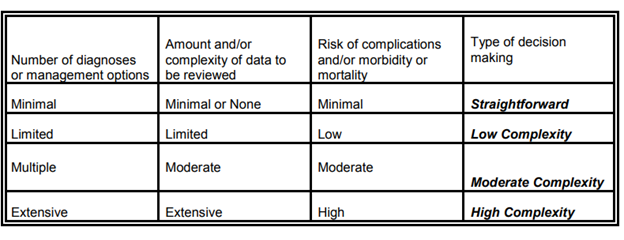
Source: 1997 Documentation guidelines for evaluation and management services.
*Medicare Carrier has changed the rules for quantifying medical decision making rules for those practicing in Delaware, Maryland, Texas, Virginia, or the District of Columbia. The above applies to the other States.
To take a deep dive into the Compliance requirements for E/M, please attend this in-person seminar Coding Evaluation and Management (E/M) From a Physician's Perspective The speaker C.J. Wolf, MD, M.Ed. has been involved in healthcare for over 20 years beginning with his years in medical school. . Apart from teaching about E/M categories, key components of E/M services he will give details about proposed 2019 changes to E/M guidelines.






